
Understanding Vulvar Eczema: Causes and Symptoms
Vulvar eczema is a skin condition that affects the vulva, the outer part of the female genitalia. It can cause discomfort and irritation, and understanding its causes and symptoms is crucial for effective management.
Causes of Vulvar Eczema
Vulvar eczema can be caused by various factors, including allergic reactions to certain products such as soaps, detergents, or feminine hygiene products. Hormonal changes, such as those that occur during pregnancy or menopause, can also contribute to vulvar eczema. Additionally, skin conditions like atopic dermatitis or contact dermatitis can trigger eczema flare-ups in the vulvar area.
Symptoms of Vulvar Eczema
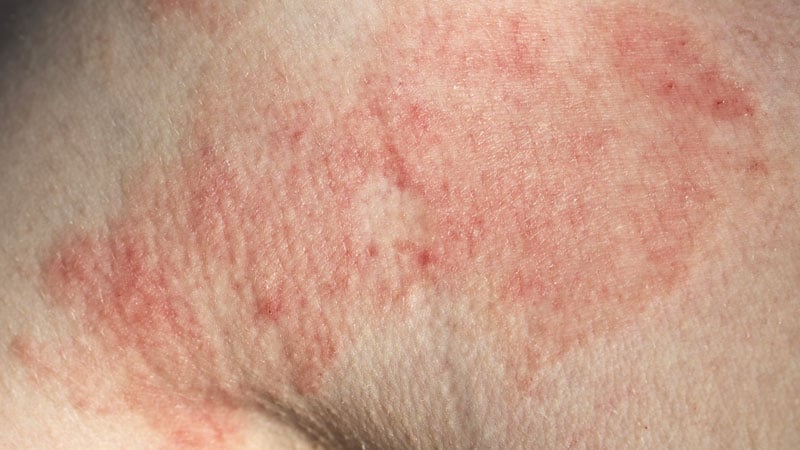
The symptoms of vulvar eczema can vary from person to person but commonly include itching, redness, swelling, and irritation in the vulvar area. Some individuals may also experience pain or a burning sensation, especially during urination or sexual intercourse. In severe cases, vulvar eczema can cause skin thickening, cracking, or bleeding.
Diagnosis and Treatment Options
Diagnosing vulvar eczema usually involves a physical examination by a healthcare provider. In some cases, additional tests such as skin biopsies may be required to rule out other conditions. Treatment options for vulvar eczema typically include:
Topical Steroids: Topical corticosteroids are commonly prescribed to reduce inflammation and alleviate symptoms of vulvar eczema. These medications come in various strengths and formulations and should be used under the guidance of a healthcare provider.
Emollients and Moisturizers: Keeping the skin moisturized is essential for managing vulvar eczema. Emollients and moisturizers can help hydrate the skin and create a protective barrier, reducing the risk of irritation and flare-ups.
Avoiding Triggers: Identifying and avoiding triggers that exacerbate vulvar eczema symptoms is crucial for long-term management. This may involve switching to hypoallergenic or fragrance-free products, wearing breathable cotton underwear, and practicing good hygiene habits.
Anti-itch Medications: Over-the-counter or prescription anti-itch medications may provide relief from itching associated with vulvar eczema. However, these medications should be used sparingly and as directed to avoid further irritation.
Lifestyle Modifications: Making lifestyle changes such as wearing loose-fitting clothing, avoiding hot baths or showers, and practicing stress management techniques can help reduce symptoms of vulvar eczema and prevent flare-ups.
Seeking Professional Advice
If you suspect you have vulvar eczema or are experiencing symptoms such as itching, redness, or irritation in the vulvar area, it’s essential to seek professional medical advice. A healthcare provider can properly diagnose your condition and recommend an appropriate treatment plan tailored to your needs.
Maintaining Vulvar Health
In addition to medical treatment, maintaining good vulvar hygiene is essential for managing vulvar eczema. Avoid using harsh soaps or douches in the vulvar area and opt for gentle, fragrance-free cleansers instead. Pat the area dry gently after washing and avoid excessive scrubbing or rubbing, which can exacerbate symptoms.
Support and Resources
Living with vulvar eczema can be challenging, but you’re not alone. There are many support groups and resources available to help you manage your condition and connect with others who understand what you’re going through. Remember to reach out to your healthcare provider if you have any questions or concerns about your vulvar health.
Schedule Your Appointment
Ready to take control of your vulvar health and find relief from vulvar eczema symptoms? Schedule an appointment with a healthcare provider at BMA-Unleash today and start your journey toward healthier skin.